Disclaimer Notice
Articles, presentations and information are provided on this website for information and research purposes only. The Guild of Naturopathic Iridologists does not endorse individual articles.
____________________________________________
CNM, The College of Naturopathic Medicine, is one of the Guild’s Accredited Iridology Teaching Colleges. They are also members of the GNC.
They generously put some YouTube videos on free release to help both the lay person and professionals with the current viral outbreak which is being experienced throughout the world.
Please follow the links to access. For GNI members watching this is a CPD opportunity of 1 CPD per Video.
https://www.youtube.com/watch?v=psemrQGaSr8&t=1s
https://www.youtube.com/watch?v=qdVQXqOLUH0
https://www.youtube.com/watch?v=N4B7k3stft8
______________________________________________________________________________
A non-invasive diabetes diagnosis method based on novel scleral imaging instrument and AI
ABSTRACT
Type 2 diabetes mellitus is one of the most common metabolic diseases in the world. However, frequent blood glucose
testing causes continual harm to diabetics, which cannot meet the needs of early diagnosis and long-term tracking of
diabetes. Thus non-invasive adjuvant diagnosis methods are urgently needed, enabling early screening of the population
for diabetes, the evaluation of diabetes risk, and assessment of therapeutic effects. The human eye plays an important
role in painless and non-invasive approaches, because it is considered an internal organ but can be easily be externally
observed. We developed an AI model to predict the probability of diabetes from scleral images taken by a specially
developed instrument, which could conveniently and quickly collect complete scleral images in four directions and
perform artificial intelligence (AI) analysis in 3 min without any reagent consumption or the need for a laboratory. The
novel optical instrument could adaptively eliminate reflections and collected shadow-free scleral images. 177 subjects
were recruited to participate in this experiment, including 127 benign subjects and 50 malignant subjects. The blood
sample and sclera images from each subject was obtained. The scleral image classification model achieved a mean AUC
over 0.85, which indicates great potential for early screening of practical diabetes during periodic physical checkups or
daily family health monitoring. With this AI scleral features imaging and analysis method, diabetic patients’ health
conditions can be rapidly, noninvasively, and accurately analyzed, which offers a platform for noninvasive forecasting,
early diagnosis, and long-term monitoring for diabetes and its complications.
CONCLUSIONS
In summary, we have developed a non-invasive AI method to predict the risk of type 2 diabetes: We have developed a
MIL model that predicts the probability of lung cancer through scleral images taken by a specially developed instrument,
which can conveniently, quickly acquire complete scleral images in four directions, complete AI analysis within 3
minutes, without any reagent consumption, and no laboratory. The average AUC of the binary classification results of
the MIL model is 0.876, indicating that there is great potential for early screening of type 2 diabetes in regular physical
examinations or daily family health monitoring.
Our results suggest a new concept that in this innovative study, the use of deep learning to analyze scleral images can
help detect type 2 diabetes. This work supports a potential step towards the development of deep learning-based tools for
pre-screening diabetes probability assessment in outpatient clinics or diabetes screening in the community, which may
help guide further diagnostic tests or visits.
Authors:
Lv, Wenqi, Fu, Rongxin, Lin, Xue, Su, Ya, Jin, Xiangyu, et al.
SPIE 11900, Optics in Health Care and Biomedical Optics XI, 1190013 (15, October 2021); doi: 10.1117/12.2601222
Department of Biomedical Engineering, School of Medicine, Tsinghua University, Beijing 100084, P. R. China
Full Abstract: https://iridology-research.com/pdf/1190013.pdf
______________________________________________________________________________
Comparative Study on Iris Manifestations between COVID-19 Severe Cases and Non-COVID Individuals
Abstract
Aims: To compare the iris manifestations between COVID-19 positive (severe) cases and their age and gender matched non-COVID-19 individuals.
Study Design and Setting: A comparative cross sectional survey performed in Government Omandurar Medical College, Chennai
Methodology: This study was performed to compare the iris manifestations between COVID-19 positive (severe) cases (n = 119) and their age and gender matched non-COVID-19 individuals (n = 119). Iris manifestations (both right and left eyes) of all the subjects (both study and control groups) were observed at only one point in time, and was compared between the groups.
Statistical Analysis: Descriptive statistics (Frequency distribution and percentage) were performed using Microsoft excel 2010. Within-group analysis was performed using Wilcoxon Signed Ranks Test, while the between-groups (study and control) analysis was performed using Chi-square test with the use of statistical package for the social sciences, version 16. P value < 0.05 was considered as significant.
Results: The research findings in right iris showed a significant difference at p<0.05 in Inner Pupillary Border (IPB), Autonomic Nerve Wreath (ANW), Scurf Rim (SCR), Inflammatory Sign (IS) and Lung Lesion (LL), while no significant difference at p<0.05 in Pupil Size (PS), Absorption Ring (AR), Iris Constitution (IC) and Stress Ring (STR) between the study and control groups. Likewise, the results of the left iris showed a significant difference at p<0.05 in IPB, ANW, SCR, LL and STR, while no significant change at p<0.05 in PS, IC, AR and IS between the study and control groups.
Conclusion: The paper aid comparison of the iris manifestations between COVID-19 positive and their age and gender matched non-COVID-19 individuals. The findings are of broad use to the scientific and medical communities searching for safe, cost-effective diagnostic approach. The present study is important in furthering our understanding of the importance of looking into the iris for diagnostic purpose.
Authors:
- Y. Rosy Ayda
- A. Mooventhan
- M. H. Vinothkumar
- C. A. Kayelarasi
- S. Vijaykanth
- N. Manavalan
Journal of Complementary and Alternative Medical Research, Page 53-60
DOI: 10.9734/jocamr/2021/v14i130238
Full Abstract: https://iridology-research.com/pdf/Comparative_Study_on_Iris_Manifestations_between_COVID-19_Severe_Cases_and_Non-COVID_Individuals.pdf
______________________________________________________________________________
Parameters to increase the quality of iridology studies: A scoping review
ABSTRACT
Introduction
Iridology is an applied health practice whose overall aim is to better understand the constitution of an individual. There are a range of new methods which can be used to acquire and interpret images but these have not as yet been reviewed. This scoping review aims to build on previous reviews and explore publications from 2014 to 2019.
Methods
This scoping review focuses on advances in iridological research methods and equipment. It followed the PRISMA-ScR guidelines and the Joanna Briggs Institute framework. The search strategy was designed in collaboration with the health sciences librarian, the principal investigator, and the researcher’s supervisors. Six relevant databases were identified. The form created prior to data extraction was used to review each article.
Results
Twenty-three publications out of a total of ninety-three publications identified were included. Four main themes emerged: (1) five different types of equipment are currently used to capture iris images in humans, (2) three different iridology-related theoretical frameworks were incorporated into the various research designs, (3) two major software-based techniques were employed to evaluate iridological signs, and, (4) sixteen of the reviewed articles linked a specific pathology or syndromic health condition of the human body represented to the reflex iris map of the eyes.
Conclusions
Computerized technological advancements in the field of iridology have helped to improve the clarity and detail of iris images and the ability to relate iridological signs to human health. The findings of this review can guide the design and methodological choices for future iridology studies.
European Journal of Integrative Medicine
_____________________________________________________________________________
Iridology-Based Dyspepsia Early Detection Using Linear Discriminant Analysis and Cascade Correlation Neural Network
Iridology_Based_Dyspepsia_Early_Detection
A very scholarly Iridology study and evaluation from Mathematicians in Indonesia. Please click on the link below to download.
______________________________________________________________________________
FASCIA TRANSMITS MESSAGES ACTING AS SECOND NERVOUS SYSTEM
Fascia Connective Tissue
“Of nerve there is no trace. But the cell framework, the cytoskeleton might serve.” 1932’s Nobel Prize winner, Dr. Charles Scott Sherrington (1857-1952) from 1952’s Man on His Nature.
Nerves provide the means for each cell in our body to be able to communicate with every other cell in our body. Right? This is not entirely true, and this been known to be not entirely true for quite some time. For one we know that chemical mediators (we refer to at least some of these as “INFLAMMATION”) provide for communication. Then there’s our MICROBIOMES, making up part of our “ENTERIC NERVOUS SYSTEM” and also allowing cellular communication and messaging between distant tissues and organs. There’s another messaging system in your body that few people are aware of that may be equally as important (some believe even more so) — FASCIA.
Fascia researcher, cell biologist and biophysicist, DR. JAMES OSCHMAN recently quoted from a biology book that is over 60 years old (Man on His Nature), which can be seen at the top of the page. The quote pertains to the fact that despite having no nervous system, a paramecium (single cell organism) can swim like a dolphin, avoid creatures trying to eat it, find food, and mate. How is this? How can a single-celled organism do all these things without a brain or nervous system to guide it and provide messages?
And increasing amount of scientific research shows that certain cells found in the connective tissues not only communicate directly with the nervous system, but with can actually communicate with each other as well — potentially over great distances. Dr Alfred Pischinger (1899-1982) was the head of the Department of Histology and Embryology at the University of Vienna’s Medical College. In 1948 he went a step further than ANDREW TAYLOR STILL and described where the “neural” control of the EXTRA CELLULAR MATRIX (the gel-like sugars, proteins, and membranes that lie between the cells and absorb mechanical stress) came from, theorizing that this is where all disease starts — something that other equally brilliant scientists are increasingly picking up on (HERE). https://www.doctorschierling.com/blog/fascial-adhesions-proprioceptive-dysfunction-as-the-common-cause-of-disease
Dr. Oschman shows how all bodily motion — no matter how small — generates electric fields that are caused by the compression, deformation, and stretching of LIGAMENTS, TENDONS, FASCIA, BONES, and other COLLAGEN-BASED CONNECTIVE TISSUES. In nerve-like fashion these messages spread throughout the surrounding tissues like ripples on a pond, providing information to other areas of the body. And if you have followed my BLOG POSTS ON FASCIA, you already realize that these messages travel through the water-based ECM at the speed of sound in water —- 750 mph as opposed to just over 150 mph, which is the speed that nerve messages travel.
Although many others have since followed his lead, Dr. Pischinger went so far as to state that Fascia is an organ (HERE is the brand new research on this https://www.doctorschierling.com/blog/is-sciences-latest-discovery-the-interstitium-really-a-new-organ-or-is-it-something-the-fascia-research-community-has-known-about-all-along
Furthermore, he says that it is the body’s single largest organ —– the only system that touches every other system (even though most physicians will tell you that SKIN is the largest organ). Although we now know that in the human body, the nerves branch down until they touch / affect each cell in the body, we are seeing that Dr. Pischinger was not far off. Pischinger was one of the first to recognize the incredible importance of Fascia when he said over a half century ago that, “The fascia must be looked upon as a single organ, a unified whole, the environment in which all body systems function.”
University of Vermont’s DR HELEN LANGEVIN (a neurologist and endocrinologist who is also affiliated with Harvard) has shown that Fascia forms a body-wide network that functions in a nerve-like signaling capacity. Like nerves, the impulses travel by way of cells that electrically polarize and depolarize. However, it does not stop there. TISSUE REMODELING, MECHANICAL LOAD, CELLULAR DEFORMATION, POSTURAL CHANGES, and changes in motion or position (PROPRIOCEPTION), also transmit signals. These signals are altered by decreased function that is caused by things like CHRONIC PAIN or injury (or MICROSCOPIC SCAR TISSUE). Interestingly enough, Dr. Langevin keeps going. She goes as far to discuss the probability of a relationship between the Connective Tissues (Fascia) and organs / organ systems. Although the conditions needed to validate this relationship have been shown to occur in “laboratory test tubes”, it has not yet been proven in living humans.
What should you take away from all of this?
Only that properly functioning Fascia and Connective Tissues are absolutely critical to one’s overall health. We have seen doctor after doctor after doctor — brilliant men of science (Oschman, Pischinger, Ingber, Still, and numerous others) who have pushed the controversial idea that all disease arises from abnormalities in the body’s Connective Tissues (HERE or HERE). https://www.doctorschierling.com/blog/fascial-adhesions-proprioceptive-dysfunction-as-the-common-cause-of-disease. Their belief is not arising from thin air, but from decades of clinical experience and research. Maybe this is why in our clinic, we frequently get COMPLETELY AMAZING RESULTS! Ignore the Fascia and other Connective Tissues at your own peril. And for those who really like what they are seeing with fascia research, I have 160+ articles on the subject all neatly categorized into one post (HERE).
Gerd Altmann – Freiburg/Deutschland – Pixabay
https://www.doctorschierling.com/blog/fascia-acts-as-second-nervous-system?fbclid=IwAR2GCvJNDgwbJKEVQWDoDO3H17YM4TLZenlGhgHjP0kNPpK33TE7oVcZhqY
____________________________
A Number of Iridology Overviews using Bernard Jensen – Dr Morse Approach
____________________________
The Cause of all Disease: A Unified Theory
____________________________
Heart Stents Fail to Ease Chest Pain
A new study has found that while stents can be lifesaving in opening arteries in patients having a heart attack, the devices are ineffective in relieving chest pain. A procedure used to relieve chest pain in hundreds of thousands of heart patients each year is useless for many of them, researchers reported on Wednesday.
Their study focused on the insertion of stents, tiny wire cages, to open blocked arteries. The devices are lifesaving when used to open arteries in patients in the throes of a heart attack.
But they are most often used in patients who have a blocked artery and chest pain that occurs, for example, walking up a hill or going up stairs. Sometimes patients get stents when they have no pain at all, just blockages.
Heart disease is still the leading killer of Americans — 790,000 people have heart attacks each year — and stenting is a mainstay treatment in virtually every hospital. More than 500,000 heart patients worldwide have stents inserted each year to relieve chest pain, according to the researchers. Other estimates are far higher.
Several companies — including Boston Scientific, Medtronic and Abbott Laboratories — sell the devices, and inserting them costs from $11,000 to $41,000 at hospitals in the United States.
The new study, published in the Lancet, stunned leading cardiologists by countering decades of clinical experience. The findings raise questions about whether stents should be used so often — or at all — to treat chest pain.
“It’s a very humbling study for someone who puts in stents,” said Dr. Brahmajee K. Nallamothu, an interventional cardiologist at the University of Michigan.
Dr. William E. Boden, a cardiologist and professor of medicine at Boston University School of Medicine, called the results “unbelievable.”
Dr. David Maron, a cardiologist at Stanford University, praised the new study as “very well conducted” but said that it left some questions unanswered. The participants had a profound blockage but only in one artery, he noted, and they were assessed after just six weeks.
“We don’t know if the conclusions apply to people with more severe disease,” Dr. Maron said. “And we don’t know if the conclusions apply for a longer period of observation.”
For the study, Dr. Justin E. Davies, a cardiologist at Imperial College London, and his colleagues recruited 200 patients with a profoundly blocked coronary artery and chest pain severe enough to limit physical activity, common reasons for inserting a stent.
All were treated for six weeks with drugs to reduce the risk of a heart attack, like aspirin, a statin and a blood pressure drug, as well as medications that relieve chest pain by slowing the heart or opening blood vessels.
Then the subjects had a procedure: a real or fake insertion of a stent. This is one of the few studies in cardiology in which a sham procedure was given to controls who were then compared to patients receiving the actual treatment.
In both groups, doctors threaded a catheter through the groin or wrist of the patient and, with X-ray guidance, up to the blocked artery. Once the catheter reached the blockage, the doctor inserted a stent or, if the patient was getting the sham procedure, simply pulled the catheter out.
Jim Stevens, a lawyer in Troy, Mich., was about to have a stent put in, but the new study gave his cardiologist pause. He advised against inserting the stent, and Mr. Stevens concurred.
Credit Sean Proctor for The New York Times.
Neither the patients nor the researchers assessing them afterward knew who had received a stent. Following the procedure, both groups of patients took powerful drugs to prevent blood clots.
The stents did what they were supposed to do in patients who received them. Blood flow through the previously blocked artery was greatly improved.
When the researchers tested the patients six weeks later, both groups said they had less chest pain, and they did better than before on treadmill tests.
But there was no real difference between the patients, the researchers found. Those who got the sham procedure did just as well as those who got stents.
Cardiologists said one reason might be that atherosclerosis affects many blood vessels, and stenting only the largest blockage may not make much difference in a patient’s discomfort. Those who report feeling better may only be experiencing a placebo effect from the procedure.
“All cardiology guidelines should be revised,” Dr. David L. Brown of Washington University School of Medicine and Dr. Rita F. Redberg of the University of California, San Francisco, wrote in an editorial published with the new study.
Clinical guidelines in the United States say stenting is appropriate for patients with a blocked artery and chest pain who have tried optimal medical therapy, meaning medications like those given to the study patients.
But those guidelines were based on studies in which patients simply said they felt better after having stents inserted.
“It was impressive how negative it was,” Dr. Redberg said of the new study. Since the procedure carries some risks, including death, stents should be used only for people who are having heart attacks, she added.
Stents came into wide use in the 1990s and became the treatment of choice because they were less invasive than bypass surgery. But there have long been questions about their effectiveness.
A large, federally funded study with Dr. Maron as a co-principal investigator, which does not have an untreated control group, is now underway to determine whether medications can be just as effective as stenting or coronary bypass in preventing heart attacks.
In 2007, another large study led by Dr. Boden — also without an untreated control group — found stents did not prevent heart attacks or deaths from heart disease.
The explanation, researchers said, was that atherosclerosis is a diffuse disease. A few arteries might be blocked today, and then reopened with stents. But tomorrow a blockage might arise in another artery and cause a heart attack.
Relieving chest pain, though, seemed a different goal to many cardiologists. After all, the heart is a muscle, and if a muscle is starved for blood, it aches.
Many patients have coronary arteries that are 80 to 90 percent blocked. Surely opening those vessels should make the patients feel better.
Mr. Stevens was on the operating table to receive a stent through his wrist when his cardiologist, Dr. Brahmajee K. Nallamothu, had second thoughts and ended the procedure.
The idea that stenting relieves chest pain is so ingrained that some experts said they expect most doctors will continue with stenting, reasoning that the new research is just one study.
Even Dr. Davies hesitated to say patients like those he tested should not get stents. “Some don’t want drugs or can’t take them,” he said.
Stenting is so accepted that American cardiologists said they were amazed ethics boards agreed to a study with a sham control group.
But in the United Kingdom, said Dr. Davies, getting approval for the study was not so difficult. Neither was it difficult to find patients.
“There are many people who are open to research, and if you tell them you are exploring a question, people agree,” he said. Nonetheless, it took him three and a half years to find the subjects for his study.
Ethics boards at many American hospitals probably would resist, since giving such patients fake procedures “flies in the face of guidelines,” Dr. Boden said.
Placebo effects can be surprisingly powerful, said Dr. Neal Dickert, Jr., a cardiologist and ethicist at Emory University.
A few years ago, researchers — at the insistence of the Food and Drug Administration — did a study to test an invasive procedure to treat high blood pressure. The control group got a sham procedure.
The method was becoming popular in Europe, but the study found that blood pressure dropped just as much in those who had the fake treatment.
Dr. Dickert said he hoped the new stent study will show cardiologists that they need to do more studies with sham procedures.
“This may turn out to be an important moment,” he said.
But getting them underway in the United States may not be easy. Ethics boards at hospitals and universities are likely to resist, as are patients.
“It’s not just up to us,” said Dr. David Goff, director of cardiovascular sciences at the National Heart, Lung and Blood Institute.
Still, the results of the new research have at least one heart specialist rethinking his practice.
Dr. Nallamothu got an advance look at the new paper on Tuesday. Coincidentally, he had a patient, Jim Stevens, 54, a lawyer in Troy, Mich., scheduled to receive a stent that day.
Mr. Stevens had a blocked artery, but the new report gave Dr. Nallamothu second thoughts. “I took him off the table,” he said.
He explained to Mr. Stevens and his wife that he did not need a stent. “I was surprised,” Mr. Stevens said.
“But I feel better not needing it.”
Credit GJLP, CNRI, via Science Source The New York Times, 2nd November 2017
RELATED COVERAGE
MENDING HEARTS
A Sea Change in Treating Heart Attacks JUNE 19, 2015
MENDING HEARTS
Putting Stents to the Test JUNE 22, 2015
MENDING HEARTS
A New, Life-or-Death Approach to Funding Heart Research OCT. 16, 2015
____________________________
Two major studies identify ‘significant concentrations’ of mercury in the red blood cells of autistic children
Mercury is a potent neurotoxin. Even the smallest amounts can cause cumulative adverse effects. Two of the most widespread forms of mercury exposure come from the organic compounds methylmercury (found in fish) and ethylmercury, which makes up 50% of the vaccine preservative thimerosal. The Agency for Toxic Substances and Disease Registry (ATSDR) affirms that young children and fetuses are particularly sensitive to harmful mercury-related effects such as “brain damage, mental retardation, incoordination, blindness, seizures and inability to speak.” This calls into question public health authorities’ aggressive peddling of annual flu shots—many of which contain thimerosal. The influenza vaccine guidelines target all children who are at least six months of age, with two closely spaced doses recommended for very young children in their “first season of vaccination.” They also target pregnant women and women who “might” be pregnant.
Organic mercury can cross the blood-brain barrier, and numerous studies have fingered it as a major offender in increasing the risk of neurodevelopmental disorders such as autism spectrum disorder (ASD), tic disorders, delayed language and attention-deficit/hyperactivity disorder (ADHD). Shamefully, the Centers for Disease Control and Prevention (CDC) refuses to admit that mercury is an ASD risk factor. Instead, it has been left up to other researchers to continue to focus attention on the compelling relationship between mercury and ASD.
Taking stock across studies
Two 2017 studies perform a valuable service by systematically reviewing the totality of published mercury-ASD evidence that has accumulated over the past dozen or so years, in particular. The two studies both come out of Iran, and both employ a technique called meta-analysis, which is a quantitative systematic review. Meta-analytic studies seek to take a step back and draw rigorous conclusions about comparable studies as a group. A key benefit of this approach is that it can consolidate “a large, and often complex, sometimes apparently conflicting, body of literature.”
The meta-analysis approach is a very appropriate tool for taking stock of published studies that compare mercury levels in ASD individuals and healthy controls without ASD. The first meta-analysis (published in the Journal of Trace Elements in Medicine and Biology by Tina Jafari and other researchers at Iran’s Shahrekord University of Medical Sciences) focuses exclusively on mercury. The second study (published in Progress in Neuropsychopharmacology and Biological Psychiatry by Amene Saghazadeh and Nima Rezaei at the Tehran University of Medical Sciences) examines mercury along with other heavy metals such as lead. Both research teams used state-of-the-art statistical techniques to produce unbiased results.
The table below summarizes the key features of study #1 (Jafari et al.) and study #2 (Saghazadeh and Rezaei):
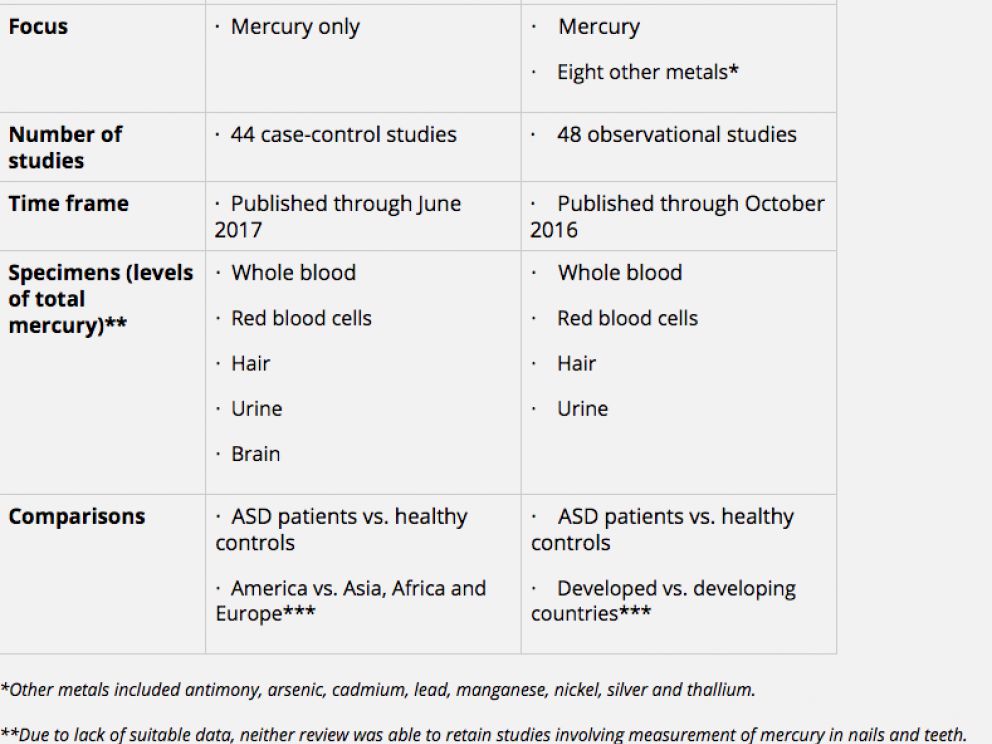
Both studies found significantly higher concentrations of mercury in the red blood cells of ASD patients versus healthy controls, and the first meta-analysis found significantly higher levels in the whole bloodof ASD patients.
The two meta-analyses examined mercury levels for each type of specimen or tissue. Both studies found significantly higher concentrations of mercury in the red blood cells of ASD patients versus healthy controls, and the first meta-analysis found significantly higher levels in the whole blood of ASD patients. (The second study also found higher levels of lead in both the red blood cells and blood of individuals with ASD, which is suggestive of possible combined or synergistic effects.)
There were no significant differences in urinary mercury levels in ASD and healthy individuals, but there were interesting findings for mercury levels in hair. In study #1, mercury concentrations were significantly lower in ASD patients compared with healthy subjects—but when the investigators analyzed their results by continent, this result held only for America but not for Asia, Africa or Europe. Similarly, study #2’s comparison of developed and developing countries found that mercury levels were significantly lower in the hair of ASD patients in developed but not developing countries—and the preponderance of developed-country studies came from the U.S.
Study #1 also affirmed significantly higher mercury levels in ASD brain tissue. However, the number of brain studies identified for the meta-analysis was very small and also somewhat unclear. The authors report pooling the results of three studies, but their reference list and table include just two studies published by Harvard researchers in 2008 and 2014, respectively. (World Mercury Project has asked the authors to clarify this discrepancy.) The 2008 study found a 68.2% increase in cerebellar mercury in autistic brain tissue (from 3.2 to 80.7 pmol g-1) compared with brain tissue of controls (from 0.9 to 35 pmol g-1), but the increase was not statistically significant. On the other hand, there was a statistically significant elevation in a key marker of oxidative stress in the ASD group that was significantly and positively correlated with elevated mercury. The 2014 study detected no difference in mercury levels but again noted elevated oxidative stress in the ASD group.
Interpreting the findings
Researchers note that a properly conducted systematic review or meta-analysis “allows the reader to take into account a whole range of relevant findings from research on a particular topic” and “establish whether the scientific findings are consistent and generalizable across populations [and] settings…and whether findings vary significantly by particular subgroups.” In addition, “mathematically combining data from a series of well-conducted primary studies may provide a more precise estimate of the underlying ‘true effect’ than any individual study.”
In this instance, the two Iranian teams used a variety of techniques to mitigate the potential weaknesses of meta-analyses. These included using multiple databases, search terms and search strategies to identify relevant studies; following established guidelines to assess the quality of each study; investigating sources of and (where appropriate) adjusting for heterogeneity; analyzing subgroup differences (i.e., the distinction between developed and developing countries); and screening for publication bias. The substantial overlap in the individual studies included in each meta-analysis and the comparability of the two teams’ findings offer a further degree of confidence in the results.
To explain the seemingly counterintuitive finding that hair mercury concentrations are lower (rather than higher) in ASD patients versus healthy individuals, Jafari et al. point to the evidence that those with ASD have impaired detoxification pathways and mechanisms.
As a result, ASD individuals retain mercury inside the cells rather than being able to effectively excrete it through the hair, stool or urine. The Iranian authors do not delve into the question of why ASD patients in developed (primarily U.S.) versus developing countries are less likely to excrete mercury and more likely to retain a heavy body burden. However, one conspicuous factor that differentiates the U.S. from other developed countries (as well as the rest of the world) may help explain this result: the U.S. promotes a far more burdensome vaccine schedule, laden with heavy metals such as thimerosal and aluminum, and annually insists that moms accept thimerosal-containing flu vaccines for themselves and their young children.
Moreover, some common flu vaccines contain the emulsifier polysorbate 80, which disrupts the blood-brain barrier and helps create an extremely effective delivery system for escorting neurotoxic ethylmercury and other heavy metals straight to the brain.
Research by Burbacher and colleagues compared blood and brain mercury levels in monkeys exposed to methylmercury and ethylmercury. That work showed that ethylmercury, in particular, goes to the brain, gets metabolized into even more toxic inorganic mercury and remains in the brain for years. Moreover, some common flu vaccines contain the emulsifier polysorbate 80, which disrupts the blood-brain barrierand helps create an extremely effective delivery system for escorting neurotoxic ethylmercury and other heavy metals straight to the brain.
Unfortunately, the majority of published studies only measure total mercury, and very few have examined brain tissue. This makes it challenging to zero in on the specific effects and mechanisms associated with exposure to ethylmercury. Given young children’s widespread exposure to ethylmercury in vaccines, there is no excuse for failing to address this research gap—and even less excuse for failing to remove thimerosal from all vaccines.
Courtesy: Nexus
____________________________
Video Presentation Holistic View of The Liver
– by Matthew D’haemer ND
A fascinating video presentation for practitioners on using iridology and energy healing for Liver issues as presented at the 19th Annual Symposium in April 2016..
____________________________
Hydrotherapy – by Abigail Francis and Roger Gross
We are grateful to Abigail and Roger for offering us the opportunity to upload their presentation on Hydrotherapy which was recently presented at the GNI Symposium in April 2016. It contains much up to date information on Hydrotherapy and draws from their visits to the Germany Kneipp site. There is a 4th section yet to update but there is much to go on for the moment. Enjoy!
HYDROTHERAPYGNI042016 Part
1HYDROTHERAPYGNI042016 Part
2HYDROTHERAPYGNI042016 Part 3
____________________________
Stress and The Liver Presentation Stress and the Liver – by Hakim M. Salim Khan, M.D. (M.A.), M.H., D.O., F.G.N.I.
____________________________
Cereal Concerns?
– by Gabi Heyes

photo credit: Bob.Fornal via photopin cc
Question: The safety of cereal was recently brought to my attention in the book Nourishing Traditions. Is cereal safe?
Answer: There are two unpublished studies regarding the safety of cereal, one involving puffed wheat and the other involving corn flakes. Both of the studies were performed on laboratory rats. The first experi- ment had results that are quite startling, involving dysfunction of the pancreas, liver, kidneys and eventually death. The sec- ond experiment had neurologi- cal and psychological outcomes such as schizophrenia, convul- sions, aggression and death.
____________________________
Foods for arthritis relief
– by Georgie O’Connor
There are lots of fabulous foods to choose from that will provide oodles of phytonutrients, antioxidants and anti-inflammatory compounds, such as pears, apples, berries, spinach, carrots and sweet potatoes…Two
to three portions of oily fish a week such as salmon, mackerel or sardines will provide the necessary essential fat, omega-3, that will ensure any inflammatory response is appropriate. If you’re vegetarian, use ground flaxseed or chia seeds. Onions, garlic, turmeric and ginger will add depth and zing to each and every meal and pack a powerful anti-inflammatory punch. You can also use ginger to flavour teas or just steep it in hot water with lemon for a refreshing alternative to regular tea. Consider increasing your consumption of green tea, to keep the anti-inflammatory nutrients coming between meals…. read more
____________________________
Fatigue & Iridology Video Presentation
– by Matthew D’haemer ND
A fascinating video presentation for practitioners on using iridology for cases with energy problems and fatigue… view video here
____________________________
Thinking of studying naturopathy – but do you know what it is?
– by Jackie Day ND, DNI, MH, FGNI

photo credit: Creativity+ Timothy K Hamilton via photopin cc
It’s not nutritional therapy and it’s not functional medicine: or is it? Naturopath Jackie Day, ND, MH, NI, FGNI, FNNA, MAMH, chair of the General Naturopathic Council, explains the scope of modern naturopathic practice – and introduces a new opportunity for qualified practitioners to earn an ND.
Sometimes you get an answer you didn’t bargain for. When preparing this article I asked several people “What does a naturopath do?” A response I didn’t see coming was “Aren’t they all hippytrippy?” So that’s who all those people ramping through the muddy fields at the Glastonbury Festival are. My question was a serious one, because in the UK the huge benefits f consulting a naturopath seem to be poorly understood, but why?… read more
Naturopathic assessment – investigating biochemical, structural and emotional integrity
– by Jackie Day ND, DNI, MH, FGNI
photo credit: The Infatuated via photopin cc
“My GP thought it was hyperthyroidism. A week later she confirmed it was an autoimmune disorder called Graves Disease. I felt so ill, I didn’t think this could happen to me.”
Sarah was a busy working mother of two young children in her mid-forties. Her stressful job as a consultant carried a great deal of responsibility. She would arrive home at 19.15, get the children ready for bed and then she’d work again, feeling that if she didn’t put in this extra time it compounded the stress the next day. At times her digestive system felt so locked up that she couldn’t eat and felt nauseous. She started to become breathless easily and people thought she was unfit, though previously she’d been a keen runner. By August 2010 she felt she couldn’t cope any longer and ended her contract in November…. read more
Naturopathic Identification of a Life-Threatening Condition
– by Angela Bradbury D.Hom., MBRI, FGNI, ND, MAMH, FICNM
Eighteen-year-old Sam had been labelled ‘a malingerer’ by the medical profession. He had been offered a place at university to study Economics and Politics but over the period of a few months he had become increasingly unwell, with severe stomach pain. When I met him, he was on the verge of losing his place at university because he was unlikely to be well enough to commence his studies.
Repeated medical investigations, including a gastroscopy and tests for Helicobacter pylori had been carried out as a stomach ulcer had been suspected, but each test came back negative, and there was no suspicion of gall-stones. Antacids proved to be of no help whatsoever. His pain was an intense burning sensation that frequently was so bad that he needed to lie down…. read more
.
Eat Right & Be Slim
– by Hakim M. Salim Khan, M.D. (M.A.), M.H., D.O., F.G.N.I.
Natural medicine, especially Tibb, takes a genuinely holistic view of food and health. The human being at the centre of the discussion is classified by their unique temperament and body type (mizaj). It also recognises that each person metabolizes food in their own specific way. Being over-weight or suffering obesity is an indication of your imbalance from this natural temperament.
Modern nutrition classifies foods by their material and chemical forms hence grouped into proteins, carbohydrates, fats, vitamins & minerals. Although this grouping provides us with some information in practice, apart from a few benefits, this simplistic and artificial classification is not much of use, therefore ignoring the most important factors: the human being and their individuality… read more
.
The Naturopathic Assessment
– by Jackie Day ND, DNI, MH, FGNI
All too often digestive problems are misdiagnosed. An accurate assessment of these conditions can bring not just rapid relief of longstanding symptoms but, as this naturopathic case study shows, much wider health benefits.
Sally had spent over half her 62 years plagued by increasing food and chemical allergies. The almost immediate reaction is swelling of her fingers, causing the skin to burst open, leaving painful cuts; hydrocortisone cream and dressings provide limited relief. She had almost come to terms with having to put up with allergies for the rest of her life so her reason for a naturopathic consultation had more to do with tiredness, skin rashes, gall-bladder gravel, and low immunity… read more
.
.
Integrated Naturopathy – homeopathy, herbs and nutrition
– by Angela Bradbury D.Hom., MBRI, FGNI, ND, MAMH, FICNM
Anne, aged 70, had a considerably overloaded gall-bladder. Her medical specialists were reluctant to treat her surgically because of high blood pressure and an inherent cardiac weakness. She was also dramatically susceptible to reactions from drugs. Hence the medical referral, my hands not being tied, and the bonus of medical monitoring.
Anne is a retired nurse who is stoically stubborn with a great sense of humour. Although born and bred in Jamaica, she had trained and worked in the UK all her working life. Partly thanks to her Caribbean upbringing, Anne taught me a lot. For example, when I explained… read more
..
Making Friends with Food
– by Hakim M. Salim Khan, M.D. (M.A.), M.H., D.O., F.G.N.I.
It is through proper use of food and good digestion that a person builds and revitalises their self and body. In order to have and maintain the right weight a person needs to have a positive and healthy relationship with food. These guidelines will help you to achieve this.
.
.
SAD – Winter Blues: the ‘other’ culprit
– by Jackie Day ND, DNI, MH, FGNI
Episodes of Seasonal Affective Disorder (SAD) develop during winter and improve in spring so reduced exposure to sunlight due to shorter winter days is the usual culprit. But, if we don’t think further than ‘light’, we may miss opportunities to help sufferers. Typical symptoms being low mood and lack of energy, SAD is classified as a type of depression; the conventional treatment is likely to be antidepressants such as Prozac. Is the trigger just reduced exposure to light, or could there be other contributory factors?
Let’s look first at the sunlight connection. One theory relates to the effect light has on the hypothalamus which controls mood, appetite and sleep. In people with SAD, a lack of sunlight and a problem with certain brain chemicals inhibits the hypothalamus… read more
Weight management – a problem as old as time
– by Jackie Day ND, DNI, MH, FGNI
photo credit: Alan Cleaver via photopin cc
We all know that most people who are overweight have eaten too much, or eaten the wrong types of food, or a combination of both. But what about those people who have genuinely stuck to the dieting rules but the weight insists on sticking to them? Experts have put forward varying explanations over the years. Current theories include genetics and chronobiology.
It is accepted that some people are genetically susceptible to weight gain, though no-one is genetically doomed to obesity, they just need to follow a genetically appropriate diet and exercise regime. Nutrigenomics is the identification of genes that are involved in physiological responses to diet and the genes in which small changes, called polymorphisms, may have significant nutritional consequences. Nutrigenetics is concerned with the effects of our individual genetic variations in response to diet and other sources of nutrients. It is the study by which dietary components communicate with the genetic material and how genetic variations affect interactions between these bioactive dietary components and the health and disease potential of a person… read more
Case Studies
Naturopathic Case Study: Hypothyroid & Food Cravings
Read how a female patient diagnosed with hypothyroidism, with symptoms of headaches and lethagy, felt inspired to take control of her health through dietary. This lead to a greater sense of wellbeing and improved energy levels… read more
.
Naturopathic Care for Type 2 Diabetes
A study reported on the reasons for the successful diabetes self-care approaches provided by Naturopathic practitioners. Although this particular study focused on type 2 diabetes, the naturopathic approach is consistent. Elements common to the success of the naturopathic approach were stated to be… read more
.
Naturopathic Case Study: Chronic Fatigue
A mother of two children with debilitating chronic fatigue decides to consult a naturopath for her condition. She learns that her strict vegan diet may need adjusting in order to help promote healing of her condition… read more
.
Naturopathic Case Study: Depression, Anxiety, Panic Attacks
A mother suffers from depression, anxiety and panic attacks after escaping a violent relationship. Through dietary changes, homeopathy, herbs and EFT she managed to overcome her condition… read more
.






